Advancing Rural Health: Addressing Market Challenges
As we begin our September blog series on Advancing Rural Health, it’s helpful to think about the challenges faced by healthcare providers and patients in America’s small-town communities. As shown in the chart below, rural Americans experience a unique combination of factors that create disparities in healthcare not found in urban areas. Market forces such as changing demographics, continued provider shortages, governmental influences and rapidly advancing technologies are changing healthcare delivery. Rural hospitals and care providers encounter additional obstacles with regard to disparate socioeconomic factors, geographical location, consumer health and lifestyle behaviors, and aging patient populations with higher-than-average rates of chronic illness.
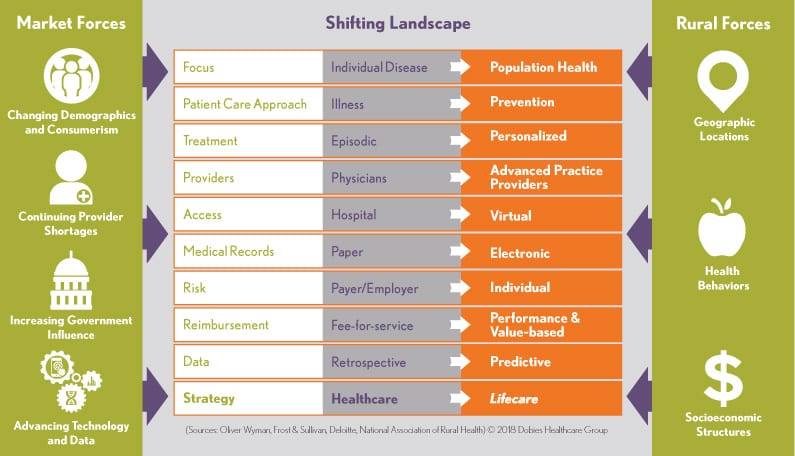
In its 2015 Policy Brief on Population Health in Rural Communities, the National Rural Health Association (NRHA) states that, “access to high-quality healthcare is a key component in supporting a healthy community … one of the reasons that rural hospitals, rural clinics and [rural community health centers] are instrumental to the overall wellbeing of rural communities.” However, citing the County Health Rankings Model from the University of Wisconsin Population Health Institute (a Robert Wood Johnson Foundation program), the NRHA brief also noted that access and quality account for only about 20 percent of the overall determinants of population health. Health behaviors such as tobacco use, diet and exercise, alcohol and drug use, and sexual activity account for 30 percent, while the physical environment affects another 10 percent. The remaining population health determinants (40 percent) are impacted by a complex tapestry of social circumstances, behavior patterns, and environmental and economic factors, including education, employment, income, family and social support, and community safety.
Together, these market factors create disparities that we must address to sustain and build the health/well-being of individuals in our regions and keep our communities healthy.
Today’s rural and critical access hospitals and care providers are at the precipice of a transformational time in healthcare history, and they are embracing transformational thinking about their role in making better health possible in their local communities. Consumerism is driving a more integrated approach to health, one that is not solely focused on providing care to patients when they are sick, but also helping to keep them healthy. At Dobies Health Marketing, we envision a model that allows health to take place in local communities by engaging and inspiring an integration of health and life services. Despite the challenges associated with rural health, a more connected system of care is within reach.
In other words, we see opportunity for rural and critical access hospitals to pivot in order to sustain their presence as community-based healthcare providers, keeping healthcare local. As leaders of a strategy-first healthcare marketing firm, my colleagues and I have been sharing insight with our rural and critical access hospital clients about how increased consumer knowledge and other market forces are driving substantial change in healthcare delivery. Such change requires greater communication and collaboration among all parties tasked with providing care and access to care (which isn’t always medical). At the core of this evolution is the need to keep people healthy throughout their lives, not simply treat them when they are sick.
Advancing Rural Health: Addressing Market Challenges - Click To TweetHospital leaders who understand these market conditions will:
- Seek resources to help you transform their organizations
- Pivot to accommodate the market forces at play
- Prepare today for the changes already underway, as well as those still to come
- Change your local market position to make better health possible
- Reinvent your brand to connect with consumers, long before they become patients
- Transform from a model of hospital care to an integrated community-wide system of health and life services
- Build collaborative relationships with community partners to weave together an integrated health and life system that inspires better health
If you are a rural or critical access hospital leader with an interest in connecting with your local community to inspire better health, take a moment to discover how dhmstudio+, a strategy-first healthcare marketing service scaled for rural hospitals, aligns with your goals.
Reader Tip: I encourage you to learn from the case study examples set by our clients at Bryan Health, who have embraced and led collaborative models in the communities of their rural and critical access hospitals.
Author’s Note: Thank you for reading this article, which is Part 1 of our series on Advancing Rural Health. I encourage you to dive into the rest of the series as well, which we are rolling out throughout September:
- Part 2 – From Healthcare to Lifecare: The visionary lifecare model and how it applies to your rural health organization
- Part 3 – Promoting the Value of Primary Care: The importance of reacquainting communities with the value of primary care
- Part 4 – Seven Steps to Service Line Marketing Strategy: A data-driven process to prioritize marketing dollars for service line growth
About the Author
 Julie Amor, MHA, President and Chief Strategy Officer for Dobies Health Marketing, has 30 years of experience elevating healthcare brands. Share your thoughts with her by tweeting @DobiesGroup, connecting with us on LinkedIn, or by commenting on our Facebook page.
Julie Amor, MHA, President and Chief Strategy Officer for Dobies Health Marketing, has 30 years of experience elevating healthcare brands. Share your thoughts with her by tweeting @DobiesGroup, connecting with us on LinkedIn, or by commenting on our Facebook page.




